How to Improve Patient Adherence to Orthotic Wear
Strategies to get your patient to wear their orthosis
Are you instructing your patients when and for how long they need to wear their new orthosis? Do your patients adhere to the prescribed orthotic wear schedule as advised? Are they following your instructions? In this blog, we share the results of one study that explored this topic, and another study that offers some unique strategies that may help improve adherence to orthotic wear.
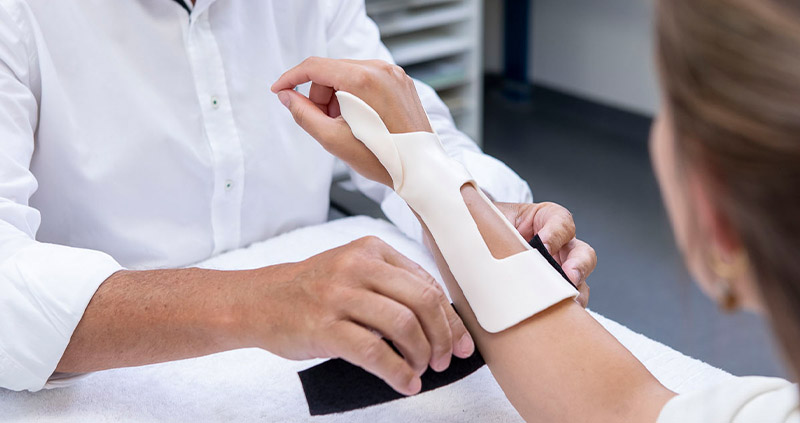
How do patients adhere to orthotic protocols?
We all hope that our patients follow our explicit directions with regard to their home exercise programs and especially any instructions regarding wearing their orthoses. However, researchers in Turkey found some different answers when they posed these questions to patients.
In their study (Savaş et al, 2020), researchers analyzed patients with acute traumatic hand tendon repairs and looked specifically at adherence to the orthotic protocol. The study included 212 consecutive patients with traumatic tendon injuries, but the final analysis included 133 patients.
Ways to evaluate patient adherence
The researchers also evaluated these patients on the Modified Hand Injury Severity Scale, the Beck Depression Inventory, and the Beck Anxiety Inventory.
Adherence was evaluated according to the Multi-Dimensional Adherence Model and rated as:
- Fully adherent
- Partially adherent
- Non-adherent
The Multi-Dimensional Adherence Model was published by the World Health Organization in 2003 and looks at socioeconomic, health care system, condition-related, treatment-related, and patient-related factors.

Method
Patients got the initial instructions to wear the prescribed orthosis 24 hours a day for three weeks and to perform specific exercises within the orthosis. They could take off their orthosis once a day for hygiene. All participants received information on the risks of not following these specific directions.
The patients received written precautions and exercises (along with photos) with encouragement to read them, or to get help with reading.
At three weeks, adherence to the orthotic wear schedule was evaluated by patient self-report:
- 33% of the patient were fully adherent
- 50% were partially adherent
- 17% were non-adherent
It is interesting to note that 92% of the patients had read the informational sheet while 7% did not read it and 1% reported that they had lost it.
A correlation between orthotic adherence and depression?
Notably, depression symptoms were found in 35% of the patient group, and 34% reported anxiety symptoms. Higher depression symptoms were associated with lower orthotic adherence.
The researchers noted many factors which could impact depression after an acute injury: many of the patients were manual laborers with low incomes and they may have worried about their loss of income and potential to work in the future. Some of the patients did not have health care insurance and may have worried about bills or the ability to provide for their families while not working. Dependency on others can also be a contributing factor for depression while in other patients, lack of adequate coping skills may be a cause.
Takeaway
This study illustrates an important aspect of our orthotic fabrication interventions. That is to say, our ability to adequately instruct the patient on orthotic wear and its importance in their recovery. It is essential to recognize patients who may benefit from additional services such as social work, counseling, and psychological interventions along with the medical and surgical care.
Can educational tools help improve adherence to orthotic wear?
Another study (Chang et al, 2019) investigated the use and patient perspective of written and online video educational tools for the conservative management of mallet finger injuries. Potential strategies to help improve adherence to orthotic wear.
The study included 61 patients (41 men and 20 women) who sustained a mallet injury. They were treated with an orthosis that immobilized the distal interphalangeal (DIP) joint.
Patients were provided with:
- A written education pamphlet and a link to an online video (both discussed the same information, but the video was specific to the type of orthosis issued)
- Verbal instructions regarding orthotic use
- Methods for self-care and cleaning
Patients’ thoughts on written and video-based instructions
At a 2-week follow-up, the patients filled out a 9-item questionnaire about the usefulness and helpfulness of the video and the written instructions.
The researchers performed statistical analysis to compare the different educational methods and to, once again, judge their usefulness and helpfulness. They also conducted analyses to study the use of written versus video instructions and check to see whether age, sex, or language were factors.
Results indicate that patients used the written instructions more than the video-based instructions. Patients did report that both were helpful and easy to understand. The helpfulness scores for the videos were significantly higher than for the written instructions. The participants also reported a preference for having access to both video and written instructions.
Takeaway
The authors of this study report that due to the importance of patient adherence to the mallet injury protocol, access to both written educational materials and online videos was of significant value.
Online instructional videos might become an important educational aid for other hand injuries as well. The authors also point out that their instructions were all written at a grade 5 level in English. Current online patient education materials, on the other hand, may actually be written at a higher level, which could be difficult for non-native speakers.
These are important considerations for enhancing patient compliance and adherence to orthotic wearing protocols in hand therapy.

Top tips to improve adherence to orthotic wear
In conclusion, we offer the following recommendations to help your patient adhere to their orthotic wearing schedule:
- Continue to check for a comfortable and well-fitting orthosis;
- Allow the patient some say in the design and/or color of the orthosis;
- Explain the purpose of the orthosis and its benefits along with the risks of non-adherence;
- Explain what activities are (not) allowed while wearing the orthosis;
- Follow up with patients regularly to encourage their adherence to the prescribed treatment plan;
- Have your patients keep a log of their orthotic wear.
A well-made orthosis is the key to successful outcomes and improved compliance. Looking to refine your splinting skills? Create a free account at the Orfit Academy and get access to a wide range of virtual courses on various splinting topics. Need help deciding which thermoplastic material to use? Contact Debby Schwartz with your questions and concerns.
Give these suggestions a try and see if they help your patients adhere to the proper orthotic wearing schedule.
References
![]()

Written by Debby Schwartz, OTD, OTR/L, CHT
Physical Rehabilitation Product and Educational Specialist at Orfit Industries America.
Debby is a certified hand therapist with over 36 years of clinical experience. She completed her Doctorate of Occupational Therapy at Rocky Mountain University of Health Professions in 2010. She has worked at Orfit Industries America as Product and Educational Specialist since 2007.
Debby is also an adjunct professor at the Occupational Therapy Department of Touro University, School of Health Sciences, and at the Occupational Therapy Department at Yeshiva University, Katz School of Science and Health in NYC. She has written many book chapters in the field of hand therapy and multiple articles for hand therapy journals, including the ASHT Times and the Journal of Hand Therapy. She has published a new textbook on orthotic fabrication together with Dr. Katherine Schofield, entitled “Orthotic Design and Fabrication for the Upper Extremity: A Practical Guide”.
![]()
If you’d like to receive the latest product updates and interesting Orfit news, subscribe to our newsletter: