Static Progressive Orthoses: The Key Basics
Effective splinting for stiff joints
The static progressive orthosis is a specific type of mobilization splint that applies a low load force to a stiff joint.
It is typically useful when treating decreased or limited upper extremity function following surgery or trauma. A common problem that is often due to decreased passive range of motion (PROM) of the joints. The static progressive orthosis will assist in improving this PROM, gradually improving the stiffness in the patient’s joint.
Here’s a brief introduction to this effective splinting technique. You’ll learn more about the basic aspects of static progressive orthoses and how you can further develop your splinting skills.

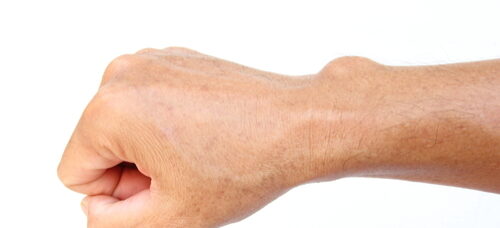
Static progressive orthoses use non-elastic components to improve passive range of motion | Left: Static Progressive Supination Orthosis in Aquafit NS. Right: Static Progressive Finger Flexion Orthosis in Orfilight.
How do static progressive orthoses work?
In essence, static progressive orthoses incorporate non-elastic components that apply force to a stiff joint or tight tissue.
The goal is to hold the joint in its “end range position” in order to improve passive range of motion. End range position refers to the maximum, pain-free, end of range for the specific joint that is stiff.
Once fabricated, a static progressive orthosis will allow the wearer to make small incremental changes in joint position as the PROM of the stiff joint slowly gives way. Patients get the instruction to constantly adjust and readjust the tension on their stiff joints.
Static progressive orthoses are typically worn 3-4 times per day for 30 minutes at a time to reap the benefits of the low-load force application
Aspects of the static progressive orthosis
Important aspects of static progressive splints include the following:
Non-elastic components
Static progressive orthoses use a non-elastic component that places tension on a stiff joint to hold it at its maximum tolerable length. The patient can make adjustments to the tension themselves.
The importance of the maximal tolerable length
In general, the orthotic design maintains the shortened tissue at its maximal tolerable length and does not stress beyond it. The longer the tissue is held at its maximum tolerable length, the more it increases in length. A successful application of a static progressive splint can be measured by gains of 5-10 degrees of passive range of motion a week.
No need to remold
The orthosis does not need to be remolded each time the patient makes progress. Rather, the original design will allow the patient to achieve full PROM from whatever starting point they began.
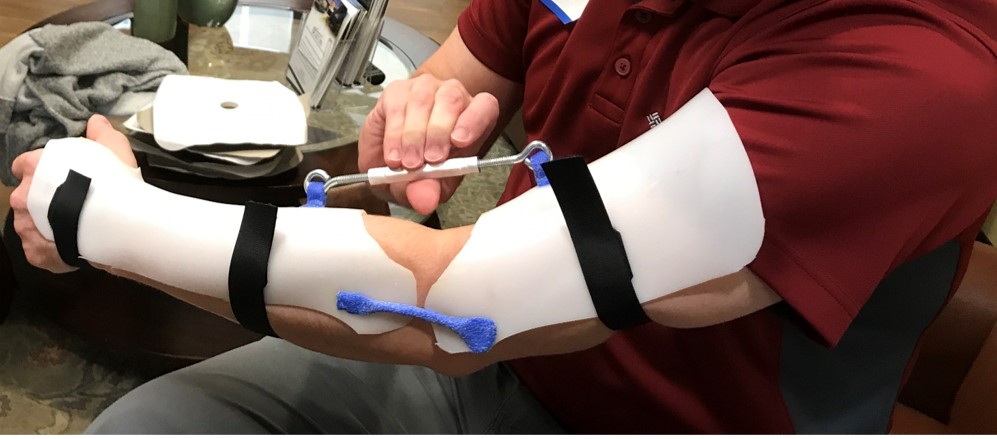
Static progressive elbow extension orthosis in Aquafit NS with Orficast hinge.
The static progressive orthosis in literature
There are many studies supporting the use of static progressive orthoses. Benefits of this intervention include the following:
- Improved range of motion without pain: there is a high tolerance for orthotic use because the patient can control the force of the tension.
- It is possible to adjust the tension force gradually, as this type of orthotic intervention takes advantage of small incremental changes in tissue length.
- The convenience of not having to remold the orthosis as the patient progresses is, of course, another great advantage.
The combination of these factors will result in improved compliance and higher patient satisfaction.
.
Learn how to fabricate
Interested in learning more about static progressive orthoses and how to fabricate them? Then be sure to register for our dedicated splinting course at the Orfit Academy, Mobilization Orthoses Part 2: Static Progressive Orthoses. Create an account or login to your account and search for the Mobilization Orthoses Part 2 course to start the course.
We offer a detailed course with fabrication videos, downloadable instructions, case studies, and a review of supporting evidence. You can even earn a certificate of attendance by paying a small fee and passing our short exam.
Enjoy and happy splinting!
![]()

Written by Debby Schwartz, OTD, OTR/L, CHT
Physical Rehabilitation Product and Educational Specialist at Orfit Industries America.
Debby is a certified hand therapist with over 36 years of clinical experience. She completed her Doctorate of Occupational Therapy at Rocky Mountain University of Health Professions in 2010. She has worked at Orfit Industries America as Product and Educational Specialist since 2007.
Debby is also an adjunct professor at the Occupational Therapy Department of Touro University, School of Health Sciences, and at the Occupational Therapy Department at Yeshiva University, Katz School of Science and Health in NYC. She has written many book chapters in the field of hand therapy and multiple articles for hand therapy journals, including the ASHT Times and the Journal of Hand Therapy. She has published a new textbook on orthotic fabrication together with Dr. Katherine Schofield, entitled “Orthotic Design and Fabrication for the Upper Extremity: A Practical Guide”.
![]()
If you’d like to receive the latest product updates and interesting Orfit news, subscribe to our newsletter:



